Understanding Pneumonoconiosis: A Guide to Dust-Related Lung Diseases
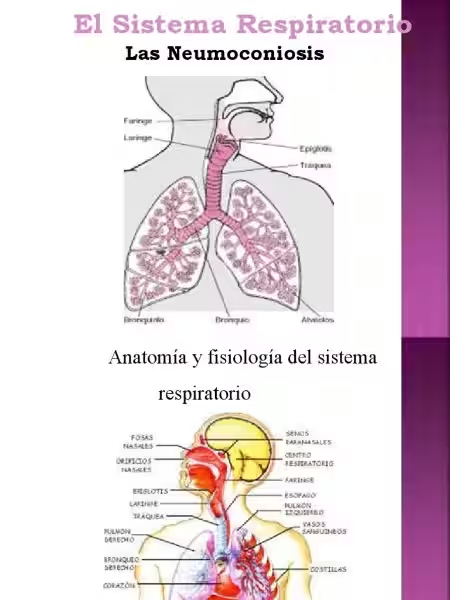
Pneumonoconiosis is a serious concern for many, especially those working in industries with high dust exposure. What exactly is it, and how can we protect ourselves? This article will explore the different types of this chronic, progressive lung disease, its symptoms, treatments, and preventative measures.
What is Pneumonoconiosis?
Pneumonoconiosis is a group of interstitial lung diseases. This means it affects the tiny air sacs (alveoli) and the supporting tissue in the lungs. The defining characteristic of pneumonoconiosis is lung inflammation and scarring, also known as pulmonary fibrosis. This scarring is a direct result of inhaling certain types of dust over extended periods. The severity and specific type of pneumonoconiosis depend entirely on the type of dust inhaled and the length of exposure.
While often linked to occupational exposure, it's crucial to understand that the condition develops slowly, meaning symptoms may not appear immediately. The body's response to the inhaled dust particles is a gradual build-up of inflammation and fibrosis that eventually compromises lung function.
Common Types of Pneumonoconiosis
Several types of pneumonoconiosis exist, each named for the specific dust causing it. The most well-known is:
- Coal Workers' Pneumoconiosis (Black Lung Disease): This arises from inhaling coal dust. A characteristic symptom is coughing up black mucus.
Other types include:
- Brown Lung Disease (Byssinosis): Caused by inhaling cotton dust.
- Pneumoconiosis from Aluminum, Barium, Beryllium, Talc, and Other Dusts: Exposure to these various industrial dusts can also lead to this condition.
It's important to note that although silicosis and asbestosis are technically forms of pneumonoconiosis, their significant impact and unique characteristics often warrant their classification as separate entities within the broader category of pulmonary fibrosis.
Distinguishing Pneumonoconiosis from Other Lung Diseases
It's vital to distinguish pneumonoconiosis from other interstitial lung diseases (ILDs). While many ILDs share the characteristic of lung scarring, their causes and treatments vary widely. These other conditions include:
- Asbestosis
- COVID-19-related pulmonary fibrosis
- Drug-induced pulmonary fibrosis
- Hypersensitivity pneumonitis
- Non-specific interstitial pneumonia
- Idiopathic pulmonary fibrosis
- Rheumatoid arthritis-associated ILD
- Systemic sclerosis-associated ILD
- Sarcoidosis
- Silicosis
Proper diagnosis requires a thorough medical evaluation to pinpoint the exact cause of the lung scarring.
Symptoms and Diagnosis of Pneumonoconiosis
Symptoms develop gradually and may initially be subtle. Common signs include:
- Persistent cough: This cough can be dry or produce mucus, which may be discolored depending on the type of dust inhaled (e.g., black in coal workers' pneumoconiosis).
- Shortness of breath (dyspnea): This is a progressive symptom, worsening as the disease advances.
- Fatigue: General tiredness and lack of energy are common complaints.
Diagnosis involves a combination of:
- Medical history: A detailed account of occupational exposures and symptoms is crucial.
- Physical examination: Listening to the lungs with a stethoscope can reveal abnormal sounds.
- Chest X-ray: This imaging test can show characteristic patterns of lung scarring.
- High-resolution computed tomography (HRCT) scan: Provides more detailed images of the lungs than a standard X-ray.
- Pulmonary function tests (PFTs): Measure lung capacity and airflow to assess the severity of lung damage.
Treatment and Management of Pneumonoconiosis
Unfortunately, there's no cure for pneumonoconiosis. Treatment focuses on managing symptoms and improving the patient's quality of life. This may include:
- Pulmonary rehabilitation: A tailored program of exercises and education to improve lung function and overall fitness.
- Oxygen therapy: Supplemental oxygen can help alleviate shortness of breath.
- Medications: May be used to manage associated conditions such as COPD or infections.
Preventing Further Progression
Smoking significantly worsens the progression of pneumonoconiosis. Smoking cessation is, therefore, paramount. Regular flu vaccinations are also recommended to prevent respiratory infections. Regular medical check-ups are essential to monitor disease progression and adjust treatment plans as needed.
Complications of Pneumonoconiosis
The progressive nature of pneumonoconiosis can lead to several complications including:
- Pulmonary hypertension: High blood pressure in the arteries of the lungs.
- Chronic obstructive pulmonary disease (COPD): A group of lung diseases that block airflow to the lungs.
- Lung cancer: Although this is not a direct result of all forms of pneumonoconiosis, the lung damage can increase susceptibility.
Prevention: The Key to Avoiding Pneumonoconiosis
The best approach to dealing with pneumonoconiosis is prevention. Minimizing dust exposure through proper workplace safety measures is crucial. This includes:
- Engineering controls: Ventilation systems, dust suppression techniques, and enclosed processes.
- Administrative controls: Limiting exposure time, job rotation, and regular medical monitoring.
- Personal protective equipment (PPE): Respirators, protective clothing, and eye protection.
By understanding the risks and implementing preventative measures, we can significantly reduce the incidence of this debilitating lung disease. Early detection and appropriate management are also critical in slowing disease progression and improving quality of life for those already affected by pneumonoconiosis.
Pneumoconiosis: Frequently Asked Questions
What is pneumoconiosis?
Pneumoconiosis is a group of lung diseases caused by inhaling certain dusts over a long period. This inhalation leads to inflammation and scarring (pulmonary fibrosis) in the lungs. The severity depends on the type of dust and the length of exposure.
What are the different types of pneumoconiosis?
The most common type is coal workers' pneumoconiosis ("black lung disease"), caused by coal dust. Other types include brown lung disease (from cotton dust) and pneumoconiosis from inhaling aluminum, barium, beryllium, talc, and other dusts. While silicosis and asbestosis are technically types of pneumoconiosis, they're often classified separately due to their severity and distinct characteristics.
How is pneumoconiosis diagnosed?
Diagnosis usually involves a combination of reviewing medical history (including occupational exposures), physical examination (listening to lung sounds), chest X-rays, and sometimes CT scans or pulmonary function tests.
What are the symptoms of pneumoconiosis?
Common symptoms include a persistent cough, shortness of breath, and fatigue. In coal workers' pneumoconiosis, coughing up black mucus is a characteristic symptom. The severity of symptoms varies depending on the stage of the disease.
Is there a cure for pneumoconiosis?
Unfortunately, there's no cure for pneumoconiosis. Treatment focuses on managing symptoms and improving quality of life through measures such as pulmonary rehabilitation, oxygen therapy, and smoking cessation.
How is pneumoconiosis treated?
Treatment aims to manage symptoms and slow disease progression. This may include pulmonary rehabilitation to improve breathing and exercise tolerance, oxygen therapy to supplement low oxygen levels, and medication to manage associated conditions like COPD.
How can I prevent pneumoconiosis?
The best prevention is avoiding exposure to harmful dusts. This might involve using appropriate respiratory protection in dusty work environments, implementing workplace safety measures, and regular medical checkups for those at risk. Smoking cessation is crucial as smoking accelerates disease progression.
Does smoking affect pneumoconiosis?
Yes, smoking significantly worsens pneumoconiosis and accelerates its progression. Quitting smoking is a vital part of managing the condition.
What are the potential complications of pneumoconiosis?
Complications can include pulmonary hypertension (high blood pressure in the lungs), chronic obstructive pulmonary disease (COPD), and lung cancer.
How is pneumoconiosis different from other lung diseases like asbestosis or silicosis?
While pneumoconiosis, asbestosis, and silicosis all involve lung scarring, they are caused by different substances and may have different symptoms and treatment approaches. Asbestosis and silicosis are often considered separately due to their unique characteristics and significant impacts. Pneumoconiosis is an umbrella term encompassing various dust-related lung diseases.
How is pneumoconiosis diagnosed? (Rephrased for clarity)
Diagnosis involves a thorough medical history, physical exam, chest X-rays, and potentially CT scans or pulmonary function tests to assess lung capacity and identify characteristic features of the disease.








